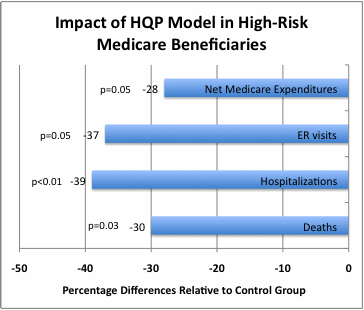
| HQP’s model of Community-based Advanced Care Management continues to demonstrate strong results. In the latest CMS report to Congress among high-risk participants, the program reduced; the rate of death -30.4% (p=0.03), hospitalizations -38.8% (p<0.01), emergency room visits -37% (p=0.05), average monthly Part A and B Medicare expenditures -$511 (-35.5%, p=0.01), and average monthly net expenditures (including program fees) -$397 (-27.6%, p=0.05). |
Though ACO’s, payment mechanisms, and control, governance, and market share concerns dominate the current health reform debate, ultimately success depends on getting better health outcomes at a lower price point. No other care coordination model has undergone as long (8+ years) or as rigorous (randomized controlled trial) an evaluation as has the HQP model. While monetary incentives may intensify motivation, they don’t, in and of themselves, provide the insight needed to understand what works … or how to effectively implement it. Perhaps it’s time we devote more attention to such issues, since they are the direct means by which we will actually achieve better health outcomes. The same cannot be said for sophisticated gainsharing financial disbursement methodologies.
A one-page summary of the HQP Community-based Advanced Care Management model and highlights of the results from the Fourth Report to Congress is available HERE.
A one-page summary of the HQP Community-based Advanced Care Management model and highlights of the results from the Fourth Report to Congress is available HERE.